AbstractPurposeThere is no optimal prognostic model for T-cell lymphoblastic lymphoma (T-LBL). Here, we discussed the predictive value of total metabolic tumor volume (TMTV) and total lesion glycolysis (TLG) measured on 18F-fluorodeoxyglucose positron emission tomography–computed tomography (PET-CT) in T-LBL.
Materials and MethodsThirty-seven treatment naïve T-LBL patients with PET-CT scans were enrolled. TMTV was obtained using the 41% maximum standardized uptake value (SUVmax) threshold method, and TLG was measured as metabolic tumor volume multiplied by the mean SUV. Progression-free survival (PFS) and overall survival (OS) were analyzed by Kaplan-Meier curves and compared by the log-rank test.
ResultsThe optimal cutoff values for SUVmax, TMTV, and TLG were 12.7, 302 cm3, and 890, respectively. A high SUVmax, TMTV, and TLG indicated a shorten PFS and OS. On multivariable analysis, TMTV ≥ 302 cm3, and central nervous system (CNS) involvement predicted inferior PFS, while high SUVmax, TLG and CNS involvement were associated with worse OS. Subsequently, we generated a risk model comprising high SUVmax, TMTV or TLG and CNS involvement, which stratified the population into three risk groups, which had significantly different median PFS of not reached, 14 months, and 7 months for low-risk group, mediate-risk group, and high-risk group, respectively (p < 0.001). Median OS were not reached, 27 months, and 13 months, respectively (p < 0.001).
IntroductionT-cell lymphoblastic lymphoma (T-LBL) is an aggressive subtype of non-Hodgkin lymphoma, characterized by male predominance and a high frequency of mediastinal tumor [1,2]. Although pediatric-derived, intensive lymphoblastic leukemia-like protocols significantly prolong survival, many patients continue to fail to achieve a response or suffer relapse [3,4]. In addition, there is no optimal prognostic model for T-LBL. Conventional markers of tumor burden, including Ann Arbor stage, International Prognostic Index (IPI), serum lactate dehydrogenase (LDH), bulky disease and bone marrow involvement, have been reported to be prognostic in limited studies [4–6]. Therefore, there remains an urgent need to identify new prognostic factors and accurate risk stratification to develop individualized treatment strategies for T-LBL.
18Fluorine fluorodeoxyglucose positron emission tomography–computed tomography (FDG PET-CT) has been adopted by the 2014 International Conference on Malignant Lymphoma imaging consensus guidelines as a powerful tool in the staging and response assessment of FDG-avid lymphoma [7]. Recently, new promising parameters measured on baseline positron emission tomography–computed tomography (PET-CT), including total metabolic tumor volume (TMTV), and total lesion glycolysis (TLG), which estimate both tumor burden and metabolism, have been shown to be significantly related to inferior progression-free survival (PFS) and/or overall survival (OS) in diffuse large B-cell lymphoma (DLBCL), primary mediastinal large B-cell lymphoma, Hodgkin lymphoma (HL), follicular lymphoma (FL), peripheral T-cell lymphoma (PTCL), and extranodal natural killer/T cell lymphoma (NKTCL) [8–15].
The current study aims to determine whether the TMTV and TLG evaluated by PET-CT are capable of predicting survival in T-LBL, and to generate a risk model for T-LBL patients to identify those with a high risk of disease relapse.
Materials and Methods1. Patients and characteristicsFrom January 2013 to December 2018, 37 patients with treatment naïve T-LBL, who underwent baseline FDG PET-CT, were included in this retrospective study. All patients were diagnosed according to the 2016 World Health Organization Classification of Tumors of Hematopoietic and Lymphoid Tissues. Response assessment was made according to The International Working Group response criteria [16].
2. PET-CT parametersAll patients underwent FDG PET-CT before the initiation of chemotherapy. PET-CT scans were performed after at least six hours of fasting. Blood glucose was required to be lower than 11.1 mmol/L before initiation. Sixty minutes after the administration of 3.7–4.4 MBq/kg of 18F-FDG, images were acquired from the skull base to the upper thighs using a delicate scanner (Siemens Biograph 64 True point PET-CT, Erlangen, Germany). Computed tomography images were acquired at 130 mAs, 130 kV, and a slice width of 8 mm per rotation performed for the attenuation correction of PET scan. Corrected emission data images were reconstructed after Fourier transformation with AWOSEM software (2 iterations, 8 subsets, 5 mm Gaussian filter).
All PET-CT scans were reviewed and computed by two board-certified nuclear medicine physicians blinded to the patient’s clinical outcome. For the target lesions of FDG tracer uptake, a standardized uptake value (SUV) of ≥ 2.5 as the contouring border was considered to represent lymphoma, as suggested by Freudenberg et al. [17]. Notably, the automatically estimated lesion boundaries were partly manually redrawn to exclude physiological cardiac activity. Dedicated software (Syngo TrueD, Siemens) automatically estimated the average and maximum SUV (SUVmean and SUVmax) and metabolic tumor volume (MTV) of each lesion, which was obtained by using an isocontour threshold method based on the 41% SUVmax method as recommended by the European Association of Nuclear Medicine [18]. The highest baseline SUVmax of all lesions was considered the SUVmax of the patient. TMTV was measured as the sum of the MTVs of all nodal and extranodal lesions. Bone marrow was included in TMTV measurement when there was focal uptake. TLG was measured as MTV multiplied by the average SUV of each lesion, and then total TLG was obtained by summing TLG of all lesions.
3. Statistical analysisReceiver-operating characteristic (ROC) analysis was used to determine optimal cutoff values for SUVmax, TMTV and TLG based on survival prediction. The characteristics of the patients were compared using Fisher’s exact test or chi-square test for discrete variables, and t test or Mann-Whitney test for continuous variables. PFS was calculated from diagnosis to the date of first disease progression, relapse, death or the date of last follow-up. OS was calculated from diagnosis to the date of death from any cause or to the date of last follow-up. Survival curves were plotted according to the Kaplan-Meier method and differences between groups were analyzed using a two-tailed log rank test. Those with a p-value less than 0.1 in the univariate regression were included into the multivariable prognostic analyses, and Cox regression with a forward LR model was used to estimate the hazard ratio (HR). All statistical analyses were performed using SPSS ver. 25.0 software (IBM Corp., Armonk, NY), and p < 0.05 was considered to be statistically significant.
Results1. Patient characteristicsThirty-seven treatment naïve T-LBL patients who underwent baseline PET-CT scans were included in this study. Among these patients, 29 patients (78.4%) were male, and the median age was 22 years old, with a range of 12–75 years. Furthermore, among these patients, 32 patients were in stage III–IV, 12 patients (32.4%) had bone marrow involvement verified by bone marrow biopsy, and 17 patients had a mediastinum bulky mass > 7.5 cm in diameter. In addition, 17 patients (45.9%) were given cyclophosphamide, vincristine, doxorubicin, and dexamethasone (Hyper-CVAD) alternating with high-dose methotrexate and cytarabine (MA) chemotherapy, while the remaining 20 patients received a modified BFM-90 regimen [3], an adapted pediatric-like acute lymphoblastic leukemia protocol. Moreover, 10 patients underwent hematopoietic stem cell transplantation after remission, which included two autologous and eight allogenic stem cell transplantations. The detailed patient characteristics are outlined in Table 1.
The median follow-up time was 26.5 months (range, 7.5 to 65 months). At the time of the analysis, 26 patients (70%) had disease progression, while 17 patients (46%) died from T-LBL. A total of six patients (19%) died within the first 6 months.
2. PET-CT parametersThe median SUVmax, TMTV, and TLG were 10.80, 383.00 cm3, and 1,644.20, respectively, with ranges of 3.70–29.70, 55.10–2,053.80 cm3, and 115.80–18,132.40, respectively. The area under the ROC curve was 0.591 (p=0.388), 0.818 (p=0.002), and 0.769 (p=0.011) for SUVmax, TMTV, and TLG, respectively (Fig. 1). The ROC curves were used to determine the optimal cutoff value for each parameter based on PFS and OS analysis. A cutoff of 12.70 (sensitivity, 46.20%; specificity, 72.70%), 302 cm3 (sensitivity, 88.50%; specificity, 72.70%) and 890 (sensitivity, 84.60%; specificity, 63.60%) was selected for SUVmax, TMTV, and TLG, respectively.
The presence of a high SUVmax (≥ 12.7) was significantly associated with a higher IPI and lower hemoglobin, while patients with high TMTV and TLG were more likely to have more than two sites of extranodal involvement. However, these three indicators were not significantly correlated with bulky disease. Comparisons of patient characteristics according to PET-CT parameters are shown in S1 Table.
3. Clinical and biological parametersBy the end of follow-up, there were 30 evaluable patients. Among them, 12 (40%) had achieved complete response, 11 (36.7%) had achieved partial response, and seven (23.3%) experienced disease progression. However, there was no difference in the overall response rate between the different PET-CT parameter groups.
The Four-year PFS and OS of the entire cohort were 23.3% and 32.2%, respectively (S2 Fig.). Patients with a high SUVmax had significantly shortened PFS and OS (median PFS, 10.5 months vs. 16.0 months; p=0.022; hazard ratio [HR], 2.54 and median OS, 13.5 months vs. 35.0 months; p=0.004; HR, 4.16). At a cutoff value of 302 cm3, 26 patients with a high TMTV experienced significantly worse outcomes, with a 3-year PFS and OS of 10.3% and 26.1% vs. 61.4% and 90.9% for patients with low TMTV (p=0.003 for PFS; HR, 5.19 and p=0.012 for OS; HR, 8.77). In addition, patients with a high TLG also had shortened PFS and OS (3-year PFS, 7.6% vs. 57.3%; p=0.004; HR, 4.53 and 3-year OS, 31.6% vs. 90.0%; p=0.003; HR, 12.24) (Fig. 2). When only patients with advanced disease were included, the prognostic value of SUVmax, TMTV, and TLG remained significant (S3 Fig). Meanwhile, central nervous system (CNS) involvement was also shown to be closely related to worse clinical outcome in the univariable analysis (median PFS, 5.0 months vs. 15.0 months; p < 0.001; HR, 8.80 and median OS, 11.0 months vs. 32.0 months; p=0.002; HR, 5.88) (Fig. 2). However, the Ann Arbor stage, IPI, presence of B symptoms, bulky disease, treatment regimens, and transplantation did not predict survival (Table 2).
Interestingly, the TMTV identified patients with earlier treatment failure. The 1-year PFS was 81.8% for patients with TMTV < 302 cm3 vs. 15.4% for those with a TMTV of ≥ 302 cm3. Among the 16 patients who progressed within one year, 87.5% had a high TMTV, compared with 57.1% of the 21 patients who remained progression-free for at least 1 year (p=0.045).
4. Combining PET-CT parameters with clinical indicatorsIn the multivariable analysis, a high TMTV (HR, 4.746; p=0.015) and CNS involvement (HR, 5.309; p=0.006) were identified as independent risk factors for PFS, while a high SUVmax (HR, 3.170; p=0.035), high TLG (HR, 9.253; p=0.039) and CNS involvement (HR, 5.880; p=0.007) predicted worse OS (Table 3).
Subsequently, we developed a risk model comprising SUVmax ≥ 12.7, TMTV ≥ 302 cm3, TLG ≥ 890, and CNS involvement, with each indicator ranking 1 score, which stratified the cohort into three risk groups: group 1, the low-risk group (n=11), which included patients with a score of 0–1; group 2, the mediate-risk group (n=14), which included patients with a score of 2; and group 3, the high-risk group (n=12), which included patients with a score of 3–4. These groups had significantly different median PFS of not reached, 14 months and 7 months, respectively (group 1 vs. group 2, p=0.060; group 1 vs. group 3, p < 0.001; group 2 vs. group 3, p=0.026). The median OS for each group were not reached, 27 months and 13 months, respectively (group 1 vs. group 2, p=0.034; group 1 vs. group 3, p=0.001; group 2 vs. group 3, p=0.020) (Fig. 3).
DiscussionThe present study revealed that high baseline SUVmax, TMTV, and TLG predict a worse outcome in T-LBL. Additionally, TMTV identifies patients at high risk of early progression. In combination with CNS involvement, these PET-CT parameters stratified T-LBL patients into three risk groups with significantly different clinical outcomes. As far as we aware, this is the largest cohort involved in the discussion of the utility of PET-CT in T-LBL.
PET-CT has been widely utilized for the staging and response evaluation of FDG-avid lymphoma [19–22]. Recently, the prognostic role of TMTV and TLG in various lymphomas has been demonstrated, including HL, DLBCL, FL, PTCL, and NKTCL. Furthermore, the combination of baseline PET-CT parameters with the Deauville score evaluated in interim and end-of-treatment PET-CT, the molecule profile, and the follicular lymphoma IPI (FLIPI) or PTCL (prognostic index for PTCL-U, PIT) score more significantly separated patient categories, than PET-CT parameters alone [13,14,23–28]. However, the utility of PET-CT has not been widely discussed and remains controversial in T-LBL due to its rarity. In the post induction phase of the German multicenter ALL (GMALL) trial, the positron emission tomography (PET) results were significantly associated with the response obtained after consolidation I [29], while in the GRAALL-Lysa study, the PET results did not predict a long-term survival [4]. Another earlier study explored the prognostic role of TMTV, TLG, and SUVmax in T-LBL, and revealed that a high SUVmax predicted a longer PFS and OS, while TMTV, TLG, and the Deauville score were not associated with survival [30]. However, there are pitfalls in this study: First, the PET-CT data were acquired from multicenter studies over a long time period with different scanners and protocols, which may have affected the stability of SUV and TMTV. Second, all patients enrolled in the study received corticosteroids before the PET-CT scan, which could influence FDG acquisition. Furthermore, the conclusion that a high SUVmax predicted a superior outcome could have resulted from the bias of oncogenic markers, and multivariate survival analysis was not performed.
TMTV is a measurement of the viable fraction of all tumor sites, and is a better predictor of survival than bulky disease. Although no correlation was found between TMTV or TLG and bulky disease, this study revealed that patients with high TMTV or TLG were more likely to have more than two sites of extranodal involvement. In the univariable survival analysis, a high SUVmax, TMTV, and TLG were significantly correlated with worse outcome, regardless of the treatment regimens and transplantation. More specifically, patients with a high TMTV had a 3-year OS of 26.1%, while those with a low TMTV had an OS of 90.1%. Furthermore, TMTV was further found to be correlated with early progression within one year, highlighting its importance in the clinical treatment of T-LBL. In addition, CNS involvement was found to be another independent indicator in the present cohort, regardless of whether CNS prophylaxis was routinely administered for all patients.
Pretherapy surrogate markers of tumor burden, including Ann Arbor stage, IPI, serum LDH, and tumor bulk, are routinely employed to stratify patients with lymphoma. However, these indicators are imperfect, and the IPI appears to have lost its prognostic value in T-LBL. In the GRAALL/Lysa study, NOTCH1/FBXW7 mutation and/or the absence of RAS/PTEN mutation/deletion were demonstrated to predict longer event-free survival and OS [4,31]. In the present study, a risk model that combined three PET-CT parameters with CNS involvement was generated, and three risk categories could be distinguished, with the high-risk group having a median PFS and OS of seven months and 13 months, respectively. Since only 37 patients were enrolled in the present cohort, there were still significant differences among groups. To the best of our knowledge, our study is the first to promote a risk model that combined PET-CT parameters with clinical factors to identify patients at high risk of early relapse or progression. However, this proposed model must be validated in a seperate large and independent cohort to confirm its prognostic value.
In addition to the baseline PET-CT parameters, the Deauville score and reductions in SUVmax, TMTV, and TLG acquired in interim PET-CT have also been demonstrated to be prognostic for HL, FL, DLBCL, and PTCL [24,26]. In the present study, 20 patients underwent PET-CT scans after induction therapy, which revealed that no correlation was found between the Deauville score or SUVmax reduction and survival (data not shown). Given the limited number of evaluable patients in present study, a larger population is warranted to obtain more solid results.
Together with the T-LBL in the present study, the importance of TMTV has also been exhibited in various other lymphomas. However, more questions have been raised regarding its clinical application: How can the most accurate method or the optimal cutoff of TMTV be defined for specific lymphoma subtypes? Is it possible to offer patients with a high TMTV more aggressive therapies, while sparing patients with low TMTV the adverse effects? Is the same drug concertation enough for patients with very different TMTV, but with the same body surface area? Is there any better combination of indicators, such as the mutation of oncogenic markers, molecule profile, circulating tumor cells, or DNA, that can identify patients at high risk of disease progression or early death?
Due to the absence of a recognized gold standard for assessing these parameters and the different machines and software used in different institutions, the determination of optimal cutoff values remains to be resolved and will require prospective validation. Similar to previous retrospective studies, our study included a small number of patients and was conducted in a single center, therefore the proposed model combining PET-CT parameters and CNS involvement requires validation in another independent data set.
To date, the present study represents the largest series of T-LBL with an analysis of PET-CT functional parameters, which revealed that SUVmax, TMTV, and TLG are significantly associated with clinical outcome. Combined with CNS involvement, these parameters are capable of precisely predicting patients at high risk of progression or relapse, although the proposed model needs to be validated in other studies.
Electronic Supplementary MaterialSupplementary materials are available at Cancer Research and Treatment website (https://www.e-crt.org).
NotesEthical Statement Informed consent for the collection of medical information was obtained from all patients. The present study was conducted according to the Helsinki declaration and was approved by the ethics committee of the First Affiliated Hospital of Zhengzhou University (Approval number: 2020-KY-409). Author Contributions Conceived and designed the analysis: Feng X, Wen X, Han X, Zhang M. Collected the data: Feng X, Wen X, Sun Z, Li X, Zhang L, Wu J, Fu X, Wang X, Yu H, Ma X, Zhang X, Xie X, Han X. Contributed data or analysis tools: Feng X, Wen X, Li L, Sun Z, Li X, Zhang L, Wu J, Fu X, Wang X, Yu H, Zhang X, Xie X, Han X. Performed the analysis: Feng X, Wen X, Ma X. Wrote the paper: Feng X, Wen X, Zhang M. Fig. 1Receiver operator characteristics analysis of maximum standardized uptake value (SUVmax) (A), total metabolic tumor volume (TMTV) (B), and total lesion glycolysis (TLG) (C). AUC, area under curve. 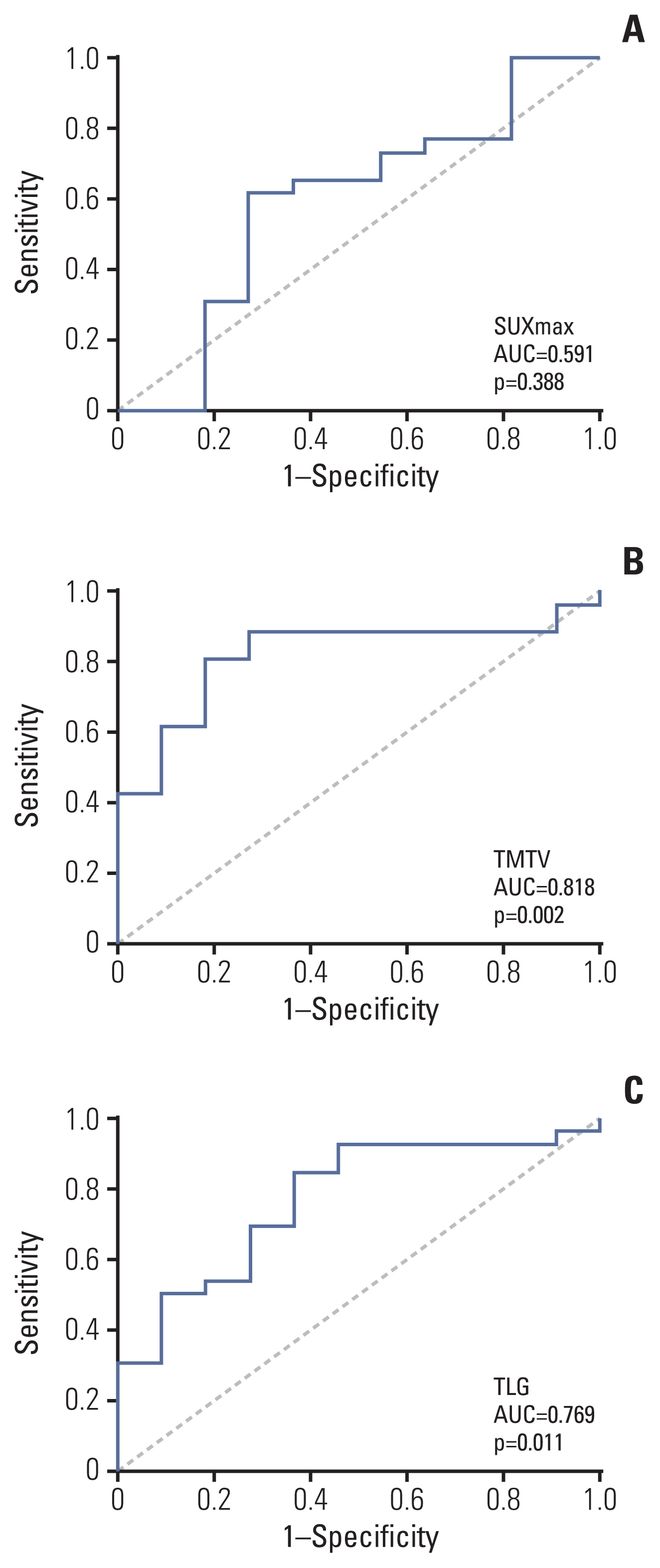
Fig. 2Kaplan-Meier estimates of progression-free survival (A, C, E, G) and overall survival (B, D, F, H) by maximum standardized uptake value (SUVmax) (A, B), total metabolic tumor volume (TMTV) (C, D), total lesion glycolysis (TLG) (E, F), and central nervous system (CNS) (G, H) involvement. 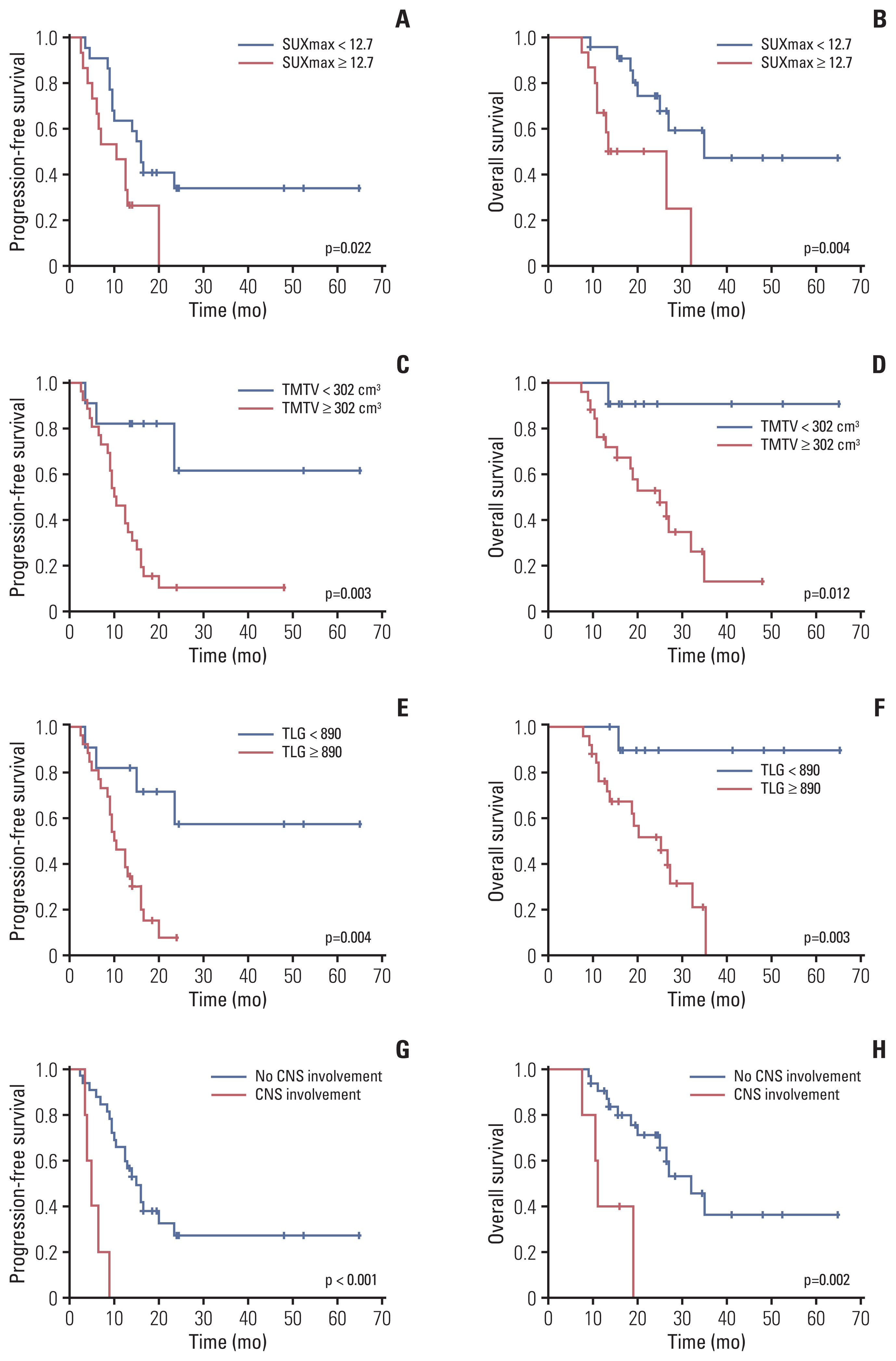
Fig. 3Progression-free survival (A) and overall survival (B) according to risk group stratification combining maximum standardized uptake value, total metabolic tumor volume, total lesion glycolysis, and central nervous system involvement. 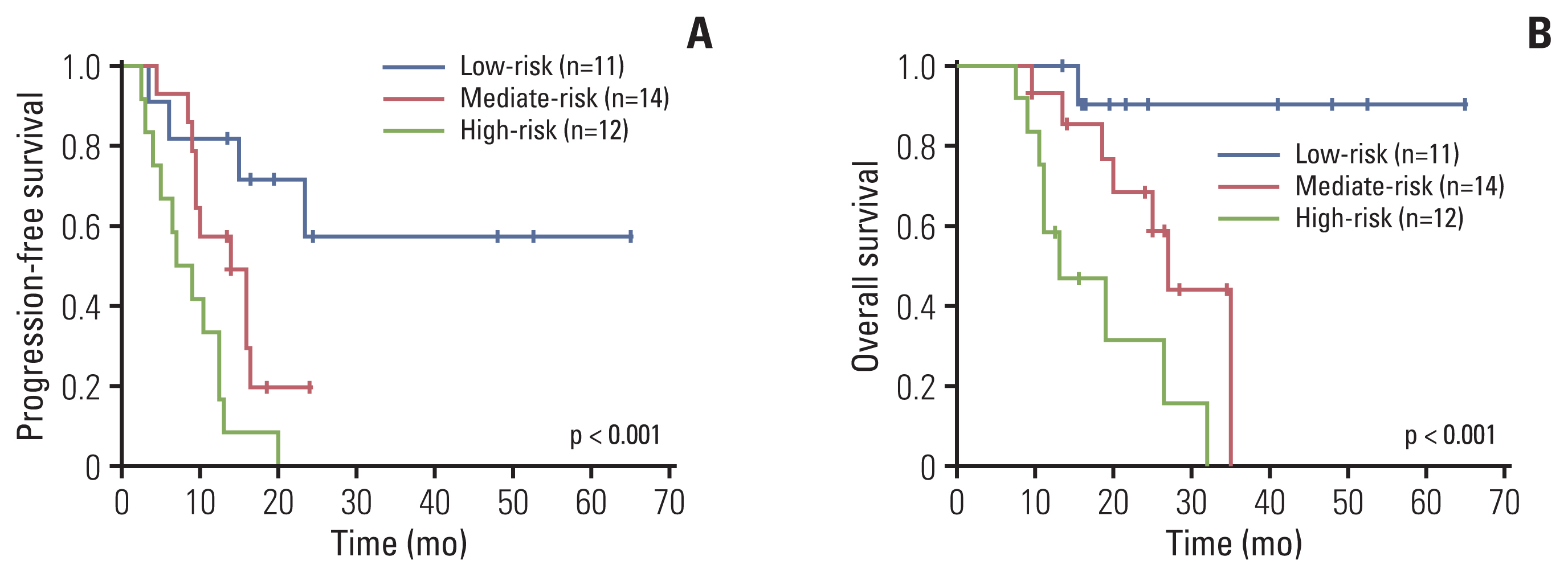
Table 1Clinical characteristics of the entire cohort Table 2Univariate analysis for prognostic factors of survival BM, bone marrow; CNS, central nervous system; ECOG, Eastern Cooperative Oncology Group; Hyper-CVAD/MA, cyclophosphamide, vincristine, doxorubicin, and dexamethasone alternating with high-dose methotrexate and cytarabine; HR, hazard ratio; IPI, International Prognostic Index; LDH, lactate dehydrogenase; NR, not reached; OS, overall survival; PFS, progression-free survival; SUVmax, standardized uptake value; TLG, total lesion glycolysis; TMTV, total metabolic tumor volume. References1. Bassan R, Maino E, Cortelazzo S. Lymphoblastic lymphoma: an updated review on biology, diagnosis, and treatment. Eur J Haematol. 2016;96:447–60.
2. Lepretre S, Graux C, Touzart A, Macintyre E, Boissel N. Adult T-type lymphoblastic lymphoma: Treatment advances and prognostic indicators. Exp Hematol. 2017;51:7–16.
3. Reiter A, Schrappe M, Ludwig WD, Tiemann M, Parwaresch R, Zimmermann M, et al. Intensive ALL-type therapy without local radiotherapy provides a 90% event-free survival for children with T-cell lymphoblastic lymphoma: a BFM group report. Blood. 2000;95:416–21.
4. Lepretre S, Touzart A, Vermeulin T, Picquenot JM, Tanguy-Schmidt A, Salles G, et al. Pediatric-like acute lymphoblastic leukemia therapy in adults with lymphoblastic lymphoma: the GRAALL-LYSA LL03 study. J Clin Oncol. 2016;34:572–80.
5. Hoelzer D, Gökbuget N, Digel W, Faak T, Kneba M, Reutzel R, et al. Outcome of adult patients with T-lymphoblastic lymphoma treated according to protocols for acute lymphoblastic leukemia. Blood. 2002;99:4379–85.
6. Thomas DA, O’Brien S, Cortes J, Giles FJ, Faderl S, Verstovsek S, et al. Outcome with the hyper-CVAD regimens in lymphoblastic lymphoma. Blood. 2004;104:1624–30.
7. Barrington SF, Mikhaeel NG, Kostakoglu L, Meignan M, Hutchings M, Müeller SP, et al. Role of imaging in the staging and response assessment of lymphoma: consensus of the International Conference on Malignant Lymphomas Imaging Working Group. J Clin Oncol. 2014;32:3048–58.
8. Kim TM, Paeng JC, Chun IK, Keam B, Jeon YK, Lee SH, et al. Total lesion glycolysis in positron emission tomography is a better predictor of outcome than the International Prognostic Index for patients with diffuse large B cell lymphoma. Cancer. 2013;119:1195–202.
9. Sasanelli M, Meignan M, Haioun C, Berriolo-Riedinger A, Casasnovas RO, Biggi A, et al. Pretherapy metabolic tumour volume is an independent predictor of outcome in patients with diffuse large B-cell lymphoma. Eur J Nucl Med Mol Imaging. 2014;41:2017–22.
10. Ceriani L, Martelli M, Zinzani PL, Ferreri AJ, Botto B, Stelitano C, et al. Utility of baseline 18FDG-PET/CT functional parameters in defining prognosis of primary mediastinal (thymic) large B-cell lymphoma. Blood. 2015;126:950–6.
11. Song MK, Chung JS, Lee JJ, Jeong SY, Lee SM, Hong JS, et al. Metabolic tumor volume by positron emission tomography/computed tomography as a clinical parameter to determine therapeutic modality for early stage Hodgkin’s lymphoma. Cancer Sci. 2013;104:1656–61.
12. Moskowitz AJ, Schöder H, Gavane S, Thoren KL, Fleisher M, Yahalom J, et al. Prognostic significance of baseline metabolic tumor volume in relapsed and refractory Hodgkin lymphoma. Blood. 2017;130:2196–203.
13. Meignan M, Cottereau AS, Versari A, Chartier L, Dupuis J, Boussetta S, et al. Baseline metabolic tumor volume predicts outcome in high-tumor-burden follicular lymphoma: a pooled analysis of three multicenter studies. J Clin Oncol. 2016;34:3618–26.
14. Cottereau AS, Becker S, Broussais F, Casasnovas O, Kanoun S, Roques M, et al. Prognostic value of baseline total metabolic tumor volume (TMTV0) measured on FDG-PET/CT in patients with peripheral T-cell lymphoma (PTCL). Ann Oncol. 2016;27:719–24.
15. Kim CY, Hong CM, Kim DH, Son SH, Jeong SY, Lee SW, et al. Prognostic value of whole-body metabolic tumour volume and total lesion glycolysis measured on 18F-FDG PET/CT in patients with extranodal NK/T-cell lymphoma. Eur J Nucl Med Mol Imaging. 2013;40:1321–9.
16. Cheson BD, Pfistner B, Juweid ME, Gascoyne RD, Specht L, Horning SJ, et al. Revised response criteria for malignant lymphoma. J Clin Oncol. 2007;25:579–86.
17. Freudenberg LS, Antoch G, Schutt P, Beyer T, Jentzen W, Muller SP, et al. FDG-PET/CT in re-staging of patients with lymphoma. Eur J Nucl Med Mol Imaging. 2004;31:325–9.
18. Meignan M, Sasanelli M, Casasnovas RO, Luminari S, Fioroni F, Coriani C, et al. Metabolic tumour volumes measured at staging in lymphoma: methodological evaluation on phantom experiments and patients. Eur J Nucl Med Mol Imaging. 2014;41:1113–22.
19. Hutchings M, Barrington SF. PET/CT for therapy response assessment in lymphoma. J Nucl Med. 2009;50(Suppl 1):21s–30s.
20. Safar V, Dupuis J, Itti E, Jardin F, Fruchart C, Bardet S, et al. Interim [18F]fluorodeoxyglucose positron emission tomography scan in diffuse large B-cell lymphoma treated with anthracycline-based chemotherapy plus rituximab. J Clin Oncol. 2012;30:184–90.
21. Barrington SF, Kirkwood AA, Franceschetto A, Fulham MJ, Roberts TH, Almquist H, et al. PET-CT for staging and early response: results from the Response-Adapted Therapy in Advanced Hodgkin Lymphoma study. Blood. 2016;127:1531–8.
22. Dupuis J, Berriolo-Riedinger A, Julian A, Brice P, Tychyj-Pinel C, Tilly H, et al. Impact of [(18)F]fluorodeoxyglucose positron emission tomography response evaluation in patients with high-tumor burden follicular lymphoma treated with immunochemotherapy: a prospective study from the Groupe d’Etudes des Lymphomes de l’Adulte and GOELAMS. J Clin Oncol. 2012;30:4317–22.
23. Malek E, Sendilnathan A, Yellu M, Petersen A, Fernandez-Ulloa M, Driscoll JJ. Metabolic tumor volume on interim PET is a better predictor of outcome in diffuse large B-cell lymphoma than semiquantitative methods. Blood Cancer J. 2015;5:e326.
24. Mikhaeel NG, Smith D, Dunn JT, Phillips M, Møller H, Fields PA, et al. Combination of baseline metabolic tumour volume and early response on PET/CT improves progression-free survival prediction in DLBCL. Eur J Nucl Med Mol Imaging. 2016;43:1209–19.
25. Cottereau AS, El-Galaly TC, Becker S, Broussais F, Petersen LJ, Bonnet C, et al. Predictive value of PET response combined with baseline metabolic tumor volume in peripheral T-cell lymphoma patients. J Nucl Med. 2018;59:589–95.
26. Cottereau AS, Versari A, Loft A, Casasnovas O, Bellei M, Ricci R, et al. Prognostic value of baseline metabolic tumor volume in early-stage Hodgkin lymphoma in the standard arm of the H10 trial. Blood. 2018;131:1456–63.
27. Cottereau AS, Lanic H, Mareschal S, Meignan M, Vera P, Tilly H, et al. Molecular profile and FDG-PET/CT total metabolic tumor volume improve risk classification at diagnosis for patients with diffuse large B-cell lymphoma. Clin Cancer Res. 2016;22:3801–9.
28. Toledano MN, Desbordes P, Banjar A, Gardin I, Vera P, Ruminy P, et al. Combination of baseline FDG PET/CT total metabolic tumour volume and gene expression profile have a robust predictive value in patients with diffuse large B-cell lymphoma. Eur J Nucl Med Mol Imaging. 2018;45:680–8.
29. Gökbuget N, Wolf A, Stelljes M, Hüttmann A, Buss EC, Viardot A, et al. Favorable outcome in a large cohort of prospectively treated adult patients with T-lymphoblastic lymphoma (T-LBL) despite slowly evolving complete remission assessed by conventional radiography. Blood. 2014;124:370.
|
|
||||||||||||||||||||||||||||||||||||||||||||||