AbstractPurpose:This study described the 2013 nationwide cancer statistics in Korea, including cancer incidence, survival, prevalence, and mortality.
Materials and Methods:Cancer incidence data from 1999-2013 were obtained from Korea National Cancer Incidence Database and followed until December 31, 2014. Mortality data from 1983-2013 were obtained from Statistics Korea. The prevalence was defined as the number of cancer patients alive on January 1, 2014 among all cancer patients diagnosed since 1999. Crude, and age-standardized and 5-year relative survival rates were also calculated.
Results:In 2013, a total of 225,343 and 75,334 Koreans were newly diagnosed and died from cancer, respectively. The age-standardized rates for cancer incidence and mortality in 2013 were 290.5 and 87.9 per 100,000, respectively. The age-standardized cancer incidence rate increased 3.1% annually between 1999 and 2013. However, the overall cancer incidence rates have decreased slightly in recent years (2011 to 2013). The age-standardized rate for all-cancer mortality has decreased 2.7% annually since 2002. Overall, the 5-year relative survival rate for people diagnosed with cancer between 2009 and 2013 was 69.4%, which represents an improved survival rate as compared with 41.2% for people diagnosed between 1993 and 1995.
IntroductionCancer is a major life-threatening disease worldwide. GLOBOCAN 2012 estimated that approximately 14.1 million patients were newly diagnosed with cancer and 8.2 million people died from cancer [1]. The global burden of cancer is expected to grow rapidly due to population growth and aging [2].
In Korea, cancer accounts for one in four deaths (27.6%) and more than 200,000 new cancer cases were diagnosed in 2012 [3]. Cancer incidence and deaths are expected to increase with increasing population aging and westernized lifestyles [4]. In addition, the economic burden of cancer in Korea increased about 1.8-fold, from $11,424 to $20,858 million, between 2000 and 2010 [5].
In this context, cancer statistics are the most important indicator to assess the national cancer burden and establish cancer prevention and control strategies. This article aims to provide nationwide cancer statistics including cancer incidence, survival, prevalence, and mortality in 2013.
Materials and Methods1. Data sourcesThe Korea Central Cancer Registry (KCCR) was established by the Ministry of Health and Welfare in 1980. Until 1998, the KCCR registered cancer cases from hospitals in order to determine cancer incidence, with increasing coverage. Since 1999, the KCCR has collected cancer incidence data nationwide by integrating a hospital-based KCCR database with data from regional cancer registry programs. The KCCR currently provides the nationwide cancer incidence, survival, and prevalence statistics annually. KCCR has been described in more detail elsewhere [6].
The KCCR built the Korea National Cancer Incidence Database (KNCI DB) from hospitals, 11 population-based registries, site-specific cancer registries, and additional medical chart review. The KNCI DB includes patient case information including age, sex, region, date of birth, date of diagnosis, primary cancer site, histological type, most valid diagnostic method, and stage. The completeness of cancer incidence data for 2013 was estimated to be 97.8% based on the method proposed by Ajiki et al. [7]. Mid-year population and cancer mortality data from 1983 to 2013 were obtained from Statistics Korea (http://kosis.kr) [8]. To ascertain vital status and calculate survival and prevalence, the KNCI DB was linked to mortality data.
2. ClassificationAll incident cancer cases were collected and registered according to the International Classification of Diseases for Oncology, 3rd edition [9]. The all cancer cases were reported according to the International Classification of Diseases, 10th edition (ICD-10) [10] and categorized into 24 cancer types.
3. Statistical analysesRates were expressed as crude and age-standardized rates (CR and ASR, respectively) per 100,000 individuals. The crude rate was calculated as the total number of incidence/mortality cases divided by the mid-year population of the specified years. The sum of the expected age-specific rates was obtained by multiplying the age-specific incidence rates among study population by the proportion of population in the corresponding age-specific groups among standard population. Next, the age-standardized incidence rates per 100,000 people were calculated as the sums of the expected age-specific rates divided by the sum of the standard population [11]. We used Segi’s world standard population to calculate the age-standardized rates [12]. Age-specific rates were also calculated for given age groups. The cumulative risk of developing cancer from birth to life expectancy were calculated using cumulative rates; that is, the sum of the age-specific rates from birth to life expectancy, as follows [13]:
Trends in incidence/mortality rates were summarized as annual percentage change (APC). APC is the average percentage change of rates and is calculated as follows [11]:
, where log(Ry)=b0+b1y,
log(Ry) is the natural log transformed age standardized rates.
y=year, b0=intercept, b1=slope
The survival duration for each cancer case was determined as the interval between the date of initial diagnosis and the date of death, date of loss of follow-up, or closing date for follow-up (December 31, 2014). Relative survival rates were calculated using the Ederer II method [14] with some minor corrections, based on an algorithm by Paul Dickman [15]. The 5-year relative survival rates were calculated as the ratios of the observed survival of the cancer patients to the expected survival of the general population, which was derived from the standard life table provided by Statistics Korea. Trends in 5-year relative survival rates were evaluated as percentage differences in 5-year relative survival rates from 1993-1995 and 2009-2013.
Prevalent cases were defined as the number of cancer patients alive on January 1, 2014 among all cancer patients diagnosed between 1999 and 2013. Limited-duration prevalences were calculated using SEER*Stat software to calculate 1-, 3-, and 5-year prevalent cases.
P-values less than 0.05 were considered statistically significant. SEER*Stat 8.2.1 (National Cancer Institute, Bethesda, MD) and SAS 9.3 (SAS Institute Inc., Cary, NC) were used to calculate the incidence, mortality, survival, and prevalence and to perform the statistical analyses.
Selected Findings1. IncidenceA total of 225,343 cases were newly diagnosed with cancer during the study period (Table 1). Of these cases, 113,744 (50.5%) were men and 111,599 cases (49.5%) were women. Thyroid cancer was the most commonly diagnosed cancer in 2013, and followed by stomach, colorectal, lung, and breast cancer in 2013. The overall cumulative risk of developing cancer from birth to life expectancy was 36.6%. However, the cumulative risk of developing cancer from birth to life expectancy was higher in men (38.3%) than in women (35.0%).
The total CR and ASR for overall cancer incidence in 2013 were 445.7 and 290.5 per 100,000, respectively (Table 2). According to sex, CRs for all sites combined were 449.9 per 100,000 in men and 441.5 per 100,000 in women. The ASRs were 316.5 and 281.8 per 100,000 in men and women, respectively. Stomach cancer (CR, 80.2 per 100,000) was the most common cancer in men, followed by colorectal (CR, 65.6 per 100,000), lung (CR, 64.0 per 100,000), liver (CR, 47.9 per 100,000), and prostate cancer (CR, 37.6 per 100,000). These five cancers accounted for 65.6% of newly diagnosed cancer in men during the study period. In contrast, thyroid cancer (CR, 134.9 per 100,000) was the most common cancer among women, followed by breast (CR, 68.2 per 100,000), colorectal (CR, 43.6 per 100,000), stomach (CR, 39.2 per 100,000), and lung cancer (CR, 27.7 per 100,000). These five cancers accounted for 71.0% of cases in women.
2. MortalityIn 2013, cancer was the most common leading cause of death in Korea (Table 3). The total number of deaths from cancer was 75,334 in 2013, accounting for 28.3% of all deaths (Table 3). According to sex, 62.5% and 37.5% of cancer deaths occurred in men and women, respectively (Table 1).
The total CR and ASR for cancer deaths were 149.0 and 87.9 per 100,000, respectively, in 2013 (Table 4). The total CR and ASR for cancer deaths per 100,000 were higher among men (ASR, 130.1) than in women (ASR, 57.5).
According to the cancer sites, lung cancer (CR, 49.5 per 100,000) was the leading cause of death in men, followed by liver (CR, 33.3 per 100,000), stomach (CR, 23.7 per 100,000), colorectal (CR, 18.4 per 100,000), and pancreatic cancer (CR, 10.3 per 100,000). The top five causes of deaths from cancer in women included lung (CR, 18.4 per 100,000), colorectal (CR, 14.0 per 100,000), stomach (CR, 12.6 per 100,000), liver (CR, 11.8 per 100,000), and breast cancer (CR, 8.8 per 100,000)
3. Trends in cancer incidence and mortality ratesThe trends in overall cancer incidence and mortality rates by sex are shown in Fig. 1. The ASR for all-cancer incidence increased 3.1% annually from 1999 to 2013 (Table 5, Fig. 1). However, in recent years, ASR for all-cancer incidence has decreased slightly, from 303.8 per 100,000 in 2011 to 290.5 per 100,000 in 2013 (APC, –2.1%). In contrast, ASR for all-cancer mortality has decreased 2.7% annually from 2002 to 2013 (Fig. 1).
The ASR for all-cancer incidence in women (APC, 5.1%; 95% confidence interval [CI], 4.6 to 5.6) has increased more rapidly than that in men (APC, 1.3%; 95% CI, 1.0 to 1.6) (Tables 6 and 7) since 1999, whereas ASR for all-cancer mortality in men (APC, –3.1%; 95% CI, –3.3 to –2.8) has decreased faster than that in women (APC, –2.2%; 95% CI, –2.5 to –1.9) since 2002 (Fig. 1).
4. Trends in cancer incidence and mortality rates by common cancer sitesBetween 1999 and 2013, ASR for thyroid cancer incidence has been most notably increased in both men (APC, 22.7%) and women (APC, 20.6%) (Tables 6 and 7). Among men, the age-standardized incidence rates of prostate (APC, 10.7%) and colorectal cancer (APC, 5.0%) have increased from 1999 to 2013, while the age-standardized incidence rates of liver (APC, –2.2%), lung (APC, –1.0%), and stomach cancer (APC, –0.8%) have decreased from 1999 to 2013 (Table 6, Fig. 2). Among women, the age-standardized incidence rates of breast (APC, 5.9%), colorectal (APC, 3.7%), and lung (APC, 1.7%) have increased from 1999 to 2013 (Table 7). However, the age-standardized incidence rates of cervical (APC, –3.9%), liver (APC, –1.8%), and stomach cancer (APC, –0.7%) in women have decreased from 1999 to 2013.
The age-standardized mortality rate of stomach cancer has decreased continuously in both sexes (Fig. 3). Although the age-standardized mortality rate of colorectal cancer increased from 1983 to 2003, the mortality rate of colorectal cancer has leveled off since 2003 in men. For women, the age-standardized mortality of colorectal cancer increased from 1983 to 2004, but the mortality rate has subsequently decreased. For both sexes, the age-standardized mortality of lung cancer increased from 1983 to 2002, and the mortality rates for lung cancer decreased. The mortality rates for uterine cancer in women and liver cancer in both sexes have continuously decreased since the mid-1990s. However, the breast cancer mortality rate in women and the prostate cancer mortality rate in men showed increasing trends during the observation period (1983-2013).
5. Age-specific incidence ratesAccording to age group, leukemia was the most commonly diagnosed cancer among children between 0-14 years of age, while thyroid cancer was the most common cancer among adolescents and young adults between 15 and 34 years of age (Table 8). For men, the incidence rate of cancer increased with age (Fig. 4A). Stomach cancer was the most commonly diagnosed cancer among men aged 35 and 64 years old, while lung cancer was the most common among elderly men aged ≥ 65 years. In contrast, thyroid cancer was most commonly diagnosed among women aged 35 and 64 years, while colorectal cancer was most common among elderly women aged ≥ 65 years. Thyroid and breast cancer showed inverted U-shaped incidence rates by age (Fig. 4B).
6. Survival ratesThe 5-year relative survival rates for all cancer combined improved remarkably in both sexes, from 41.2% in 1993-1995 to 69.4% in 2009-2013 (Table 9, Fig. 5A). After excluding thyroid cancer, the 5-year relative survival rates for all cancer still increased from 1993-1995 to 2009-2013 (Fig. 5B).
The 5-year relative survival rate in 2009-2013 for all cancer combined was 61.0% in men and 77.7% in women, respectively. The 5-year relative survival rate for thyroid cancer was over 100%, while the 5-year relative survival rates for testis, prostate, and breast cancer were over 90% in 2009-2013 for both sexes, respectively. However, the 5-year relative survival rate for pancreatic cancer was only 9.4% in both sexes in 2009-2013.
When compared to the 5-year relative survival rate for 1993-1995, prostate cancer diagnosed from 2009 to 2013 showed the most outstanding improvement, followed by stomach cancer, leukemia, ‘lip, oral cavity, and pharynx’ and colorectal cancer in men. Among women, stomach cancer diagnosed during 2009-2013 showed the greatest improvement in 5-year relative survival rates compared to those between 1993 and 1995, followed by leukemia, non-Hodgkin’s lymphoma, colorectal cancer, and kidney cancer.
7. Prevalence ratesA total of 1,370,049 cancer prevalent cases were identified on January 1, 2014 (Table 1). Of these cases, 603,524 (44.1%) were men and 766,525 (55.9%) were women. The crude and age-standardized prevalence rates for cancer overall were 2,709.8 per 100,000 individuals and 1,772.4 per 100,000 individuals for both sexes, respectively, in 2013 (Table 10). Among men, the crude and age-standardized prevalence rates for cancer overall were 2,387.1 and 1,683.6 per 100,000 individuals, respectively. Among women the rates for cancer overall were 3,032.6 and 1,944.3 per 100,000 individuals, respectively.
The five most common cancers for men were stomach (CR, 589.0 per 100,000), colorectal (CR, 449.1 per 100,000), prostate (CR, 220.5 per 100,000), thyroid (CR, 194.3 per 100,000), and liver cancer (CR, 163.0 per 100,000). In contrast, thyroid cancer was most common in women (CR, 995.9 per 100,000), followed by breast (CR, 579.3 per 100,000), colorectal (CR, 302.8 per 100,000), stomach (CR, 298.4 per 100,000), and cervix uteri cancer (CR, 181.9 per 100,000).
Analysis of the time period after cancer diagnosis revealed that thyroid cancer (23.2%) was the most prevalent cancer within 2 years after cancer diagnosis, followed by stomach (13.9%) and colorectal cancer (13.3%) (Fig. 6). Thyroid cancer (26.2%) was most prevalent for 2-5 years, followed by stomach (15.4%) and colorectal cancer (14.0%). After 5 years, stomach cancer (18.6%) was the most prevalent cancer, followed by thyroid (18.1%) and colorectal cancer (14.1%).
Notes*The Community of Population-Based Regional Cancer Registries Chang-Hoon Kim (Busan Cancer Registry, Pusan National University Hospital), Cheol-In Yoo (Ulsan Cancer Registry, Ulsan University Hospital), Heon Kim (Chungbuk Cancer Registry, Chungbuk National University Hospital), Hae-Sung Nam (Daejeon/Chungnam Cancer Registry, Chungnam National University Hospital), Jung-Sik Huh (Jeju Cancer Registry, Jeju National University Hospital), Jung-Ho Youm (Chonbuk Cancer Registry, Chonbuk National University Hospital), Moo-Kyung Oh (Kangwon Cancer Registry, Kangwon National University Hospital), Nam-Soo Hong (Daegu/Gyeongbuk Cancer Registry, Kyungpook National University Medical Center), Sun-Seog Kweon (Gwangju/Chonnam Cancer Registry, Chonnam National University Hwasun Hospital), Woo-Chul Kim (Incheon Cancer Registry, Inha University Hospital), Yune-Sik Kang (Gyeongnam Cancer Registry, Gyeongsang National University Hospital) AcknowledgmentsThis work was supported by a research grant from the National Cancer Center (No. 1610200), Republic of Korea. The authors are indebted to Korea Central Cancer Registry (KCCR)-affiliated hospitals, non-KCCR-affiliated hospitals, the National Health Insurance Service and Statistics Korea for data collection.
Fig. 1.Annual age-standardized cancer incidence and death rates by sex for all sites from 1983 to 2013 in Korea. Age standardization was based on the Segi’s world standard population. 
Fig. 2.Trends in age-standardized incidences of selected cancers by sex from 1999 to 2013 in Korea. (A) Men. (B) Women. Age standardization was based on the Segi’s world standard population. 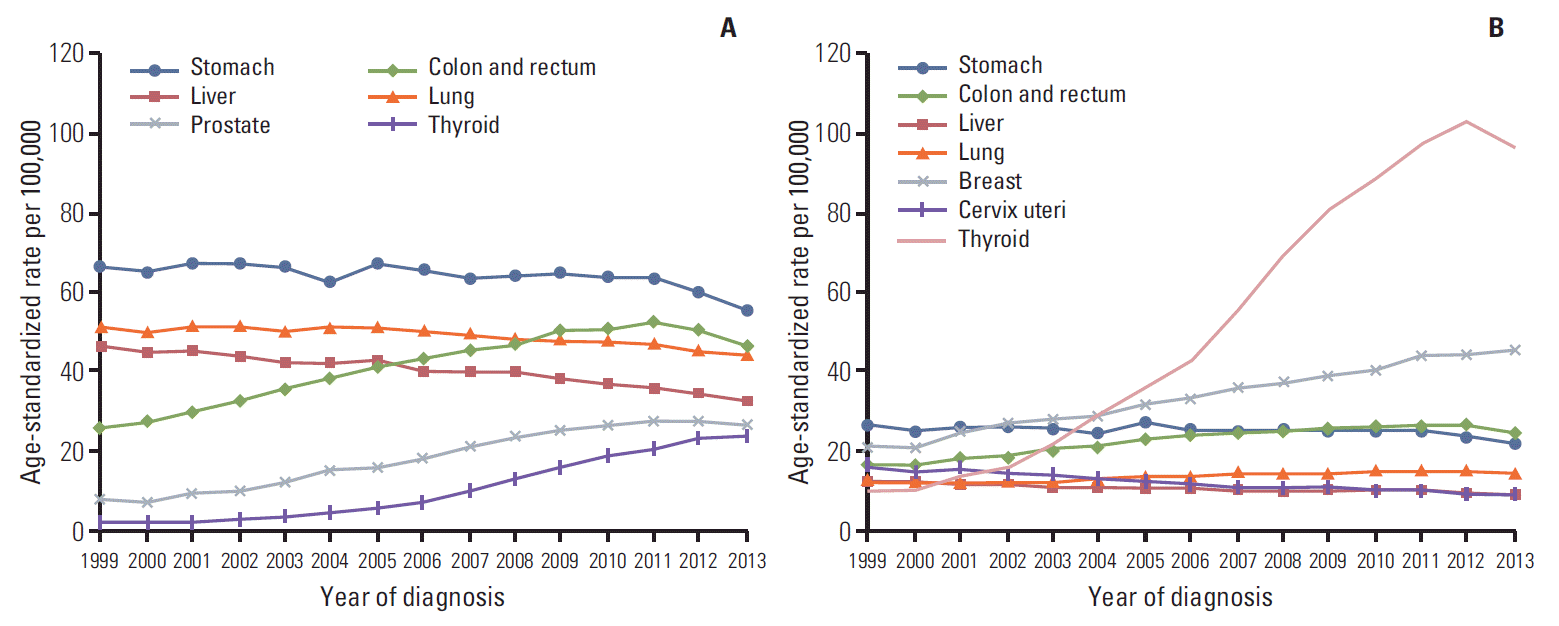
Fig. 3.Annual age-standardized cancer mortalities of selected cancers by sex from 1983 to 2013 in Korea. (A) Men. (B) Women. Age standardization was based on the Segi’s world standard population. 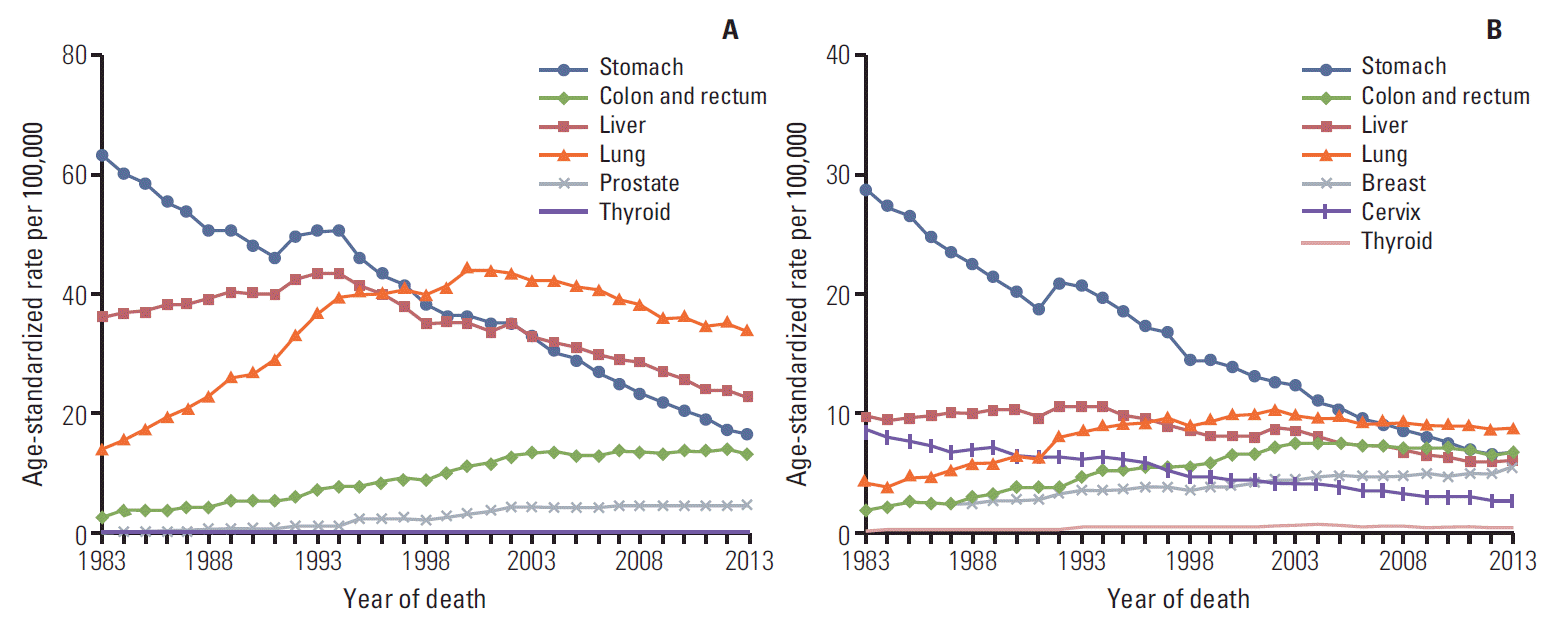
Fig. 5.Trends in relative survival by year of diagnosis from 1999 to 2013. (A) All sites for both sexes. (B) All sites except thyroid cancer for both sexes. 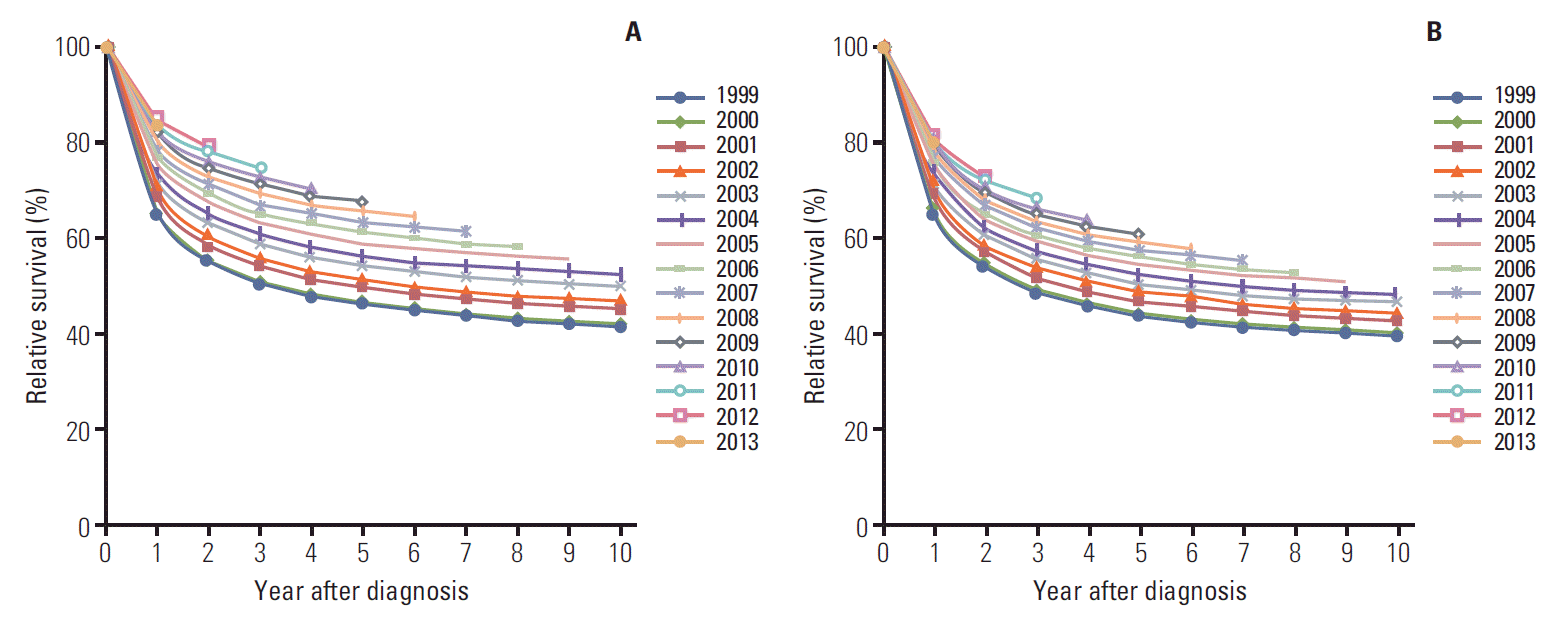
Fig. 6.Prevalence of common cancer sites by time period after cancer diagnosis. Prevalent cases were defined as the number of cancer patients alive on January 1, 2014 among all cancer patients diagnosed between 1999 and 2013. 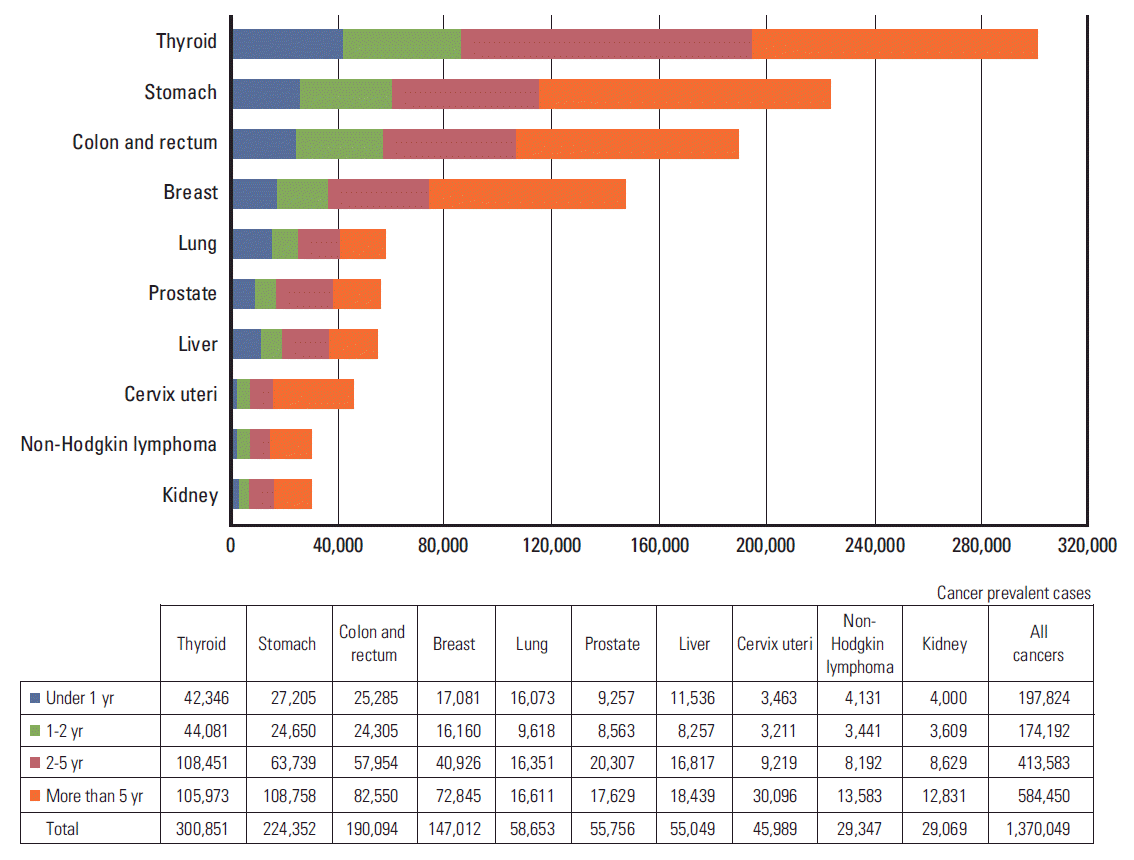
Table 1.Cancer incidence, deaths and prevalence by sex in Korea, 2013
Table 2.Crude and age-standardized cancer incidence rates by sex in Korea, 2013
Table 3.The top 10 leading causes of death in Korea, 2013
Source: Mortality Data, 2013, Statistics Korea [8]. Table 4.Crude and age-standardized cancer mortality rates by sex in Korea, 2013
Table 5.Trends in cancer incidence rates for both sexes from 1999 to 2013 in Korea
Table 6.Trends in cancer incidence rates in men from 1999 to 2013 in Korea
Table 7.Trends in cancer incidence rates in women from 1999 to 2013 in Korea
Table 8.The five common sites of cancer incidence by age group and sex in Korea, 2013 Table 9.Trends in the 5-year relative survival rates (%) by year of diagnosis from 1993 to 2013 in Korea
Table 10.Crude and age-standardized rates of cancer prevalence by sex on January 1, 2014 in Korea
a) Crude prevalence rate: number of prevalent cases divided by the corresponding person-years of observation. Prevalent cases were defined as patients who were diagnosed between January 1, 1999 and December 31, 2013 and who were alive on January 1, 2014. Multiple primary cancer cases were counted multiple times, References1. Ferlay J, Soerjomataram I, Ervik M, Dikshit R, Eser S, Mathers C, et al. GLOBOCAN 2012 v1.0. Cancer incidence and mortality worldwide: IARC CancerBase No. 11 [Internet]. Lyon: International Agency for Research on Cancer; 2013. [cited 2016 Jan 28]. Available from: http://globocan.iarc.fr
2. GBD 2013 Mortality and Causes of Death Collaborators. Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2015;385:117–71.
3. Jung KW, Won YJ, Kong HJ, Oh CM, Cho H, Lee DH, et al. Cancer statistics in Korea: incidence, mortality, survival, and prevalence in 2012. Cancer Res Treat. 2015;47:127–41.
4. Jung KW, Won YJ, Oh CM, Kong HJ, Cho H, Lee DH, et al. Prediction of cancer incidence and mortality in Korea, 2015. Cancer Res Treat. 2015;47:142–8.
5. Lee KS, Chang HS, Lee SM, Park EC. Economic burden of cancer in Korea during 2000-2010. Cancer Res Treat. 2015;47:387–98.
6. Shin HR, Won YJ, Jung KW, Kong HJ, Yim SH, Lee JK, et al. Nationwide cancer incidence in Korea, 1999~2001; first result using the national cancer incidence database. Cancer Res Treat. 2005;37:325–31.
7. Ajiki W, Tsukuma H, Oshima A. Index for evaluating completeness of registration in population-based cancer registries and estimation of registration rate at the Osaka Cancer Registry between 1966 and 1992 using this index. Nihon Koshu Eisei Zasshi. 1998;45:1011–7.
8. Statistics Korea [Internet]. Daejeon: Statistics Korea; 2015. [cited 2015 Jan 28]. Available from: http://kosis.kr
9. Fritz A, Percy C, Jack A, Shanmugaratnam K, Sobin L, Parkin DM, et al. International classification of diseases for oncology. 3rd edGeneva: World Health Organization; 2000.
10. World Health Organization. International statistical classification of diseases and related health problems. 10th revGeneva: World Health Organization; 1994.
11. Howlader N, Noone AM, Krapcho M, Garshell J, Miller D, Altekruse SF, et al. SEER cancer statistics review, 1975-2012 [Internet]. Bethesda, MD: National Cancer Institute; 2013. [cited 2015 Jan 28]. Available from: http://seer.cancer.gov/csr/1975_2012/
12. Segi M. Cancer mortality for selected sites in 24 countries (1950-1957). Sendai: Tohoku University School of Medicine; 1960.
13. Day NE. Cumulative rates and cumulative riskIn : Muir C, Waterhouse J, Mack T, Powell J, Whelan S, editors. Cancer incidence in five continents. Vol. V. IARC Scientific Publications No. 88. Lyon: International Agency for Research on Cancer; 787. p. 1011–9.
14. Ederer F, Heise H. Instructions to IBM 650 programmers in processing survival computations. Methodological note, No. 10. Bethesda, MD: National Cancer Institute; 1959.
15. Paul Dickman [Internet]. Stockholm: PaulDickman.com; 2016. [cited 2016 Jan 14]. Available from: http//www.pauldickman.com
|
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||