Real-World Study Evaluating Safety and Effectiveness of Axitinib in Korean Patients with Renal Cell Carcinoma after Failure of One Prior Systemic Therapy
Article information
Abstract
Purpose
This post-marketing surveillance (PMS) study was conducted to monitor the usage of axitinib (Inlyta) in clinical practice of Korean patients with advanced renal cell carcinoma (RCC) with disease progression during or after a prior systemic therapy in real world.
Materials and Methods
In this multicenter, observational study, patients indicated for oral axitinib 5 mg twice daily as second-line therapy for advanced RCC were followed up under routine clinical practices, and their safety and effectiveness outcomes were collected.
Results
Between 2012 and 2021, 125 patients were enrolled, and data from 111 patients were analyzed. Median age was 65 years (range, 30 to 84 years), 81% was male, and 110 (99%) had clear cell RCC. The median daily dose of axitinib was 10 mg (range, 4.36 to 15.95 mg) with a median administration period of 5.6 months (range, 15 to 750 days). Eighty-three percentage of patients experienced any grade of adverse events, 71% of which were related to study treatment, including diarrhea (36%), hypertension (21%), stomatitis (17%), decreased appetite (14%), palmar-plantar erythrodysesthesia syndrome (12%), and asthenia (11%). Most adverse events were generally well tolerated and manageable, with 13% of grade ≥ 3. Axitinib dose reduction was required in 20% of the adverse events and discontinuation in 8%. Median progression-free survival was 12.4 months (95% confidence interval [CI], 9.6 to 18.9). Objective responses were observed in 30% of patients (95% CI, 21 to 39) with 4% of complete response and 26% of partial response.
Conclusion
No new safety signal was found in the present PMS study of Korean RCC patients. Axitinib showed consistent outcomes in terms of effectiveness and safety confirming that the drug is a valid option for second-line therapy in patients with advanced RCC in a real-world setting.
Introduction
According to Korean nationwide statistics in 2018, renal cell carcinoma (RCC) is the tenth most common neoplasm with the age-standardized incidence rate of 6.3/100,000, and the incidence is rising for past decades [1]. About one-third of RCCs are diagnosed as metastatic tumors, and recurrence is common in patients treated for localized disease [2].
Most RCCs are highly vascularized and overexpress multiple growth factors, leading to the development of tyrosine kinase inhibitors against vascular endothelial growth factor receptor (VEGFR) such as sunitinib [3], pazopanib [4], and axitinib [5].
Axitinib is a potent, selective, second-generation inhibitor of VEGFR 1, 2, and 3 with a relative potency 50–450 times greater than that of the first-generation VEGFR inhibitors [6]. In the AXIS trial [5], axitinib was compared with sorafenib in patients failed to prior cytokine treatment or targeted agents (mainly sunitinib). Based on the superiority of axitinib over sorafenib [7], axitinib was approved by the Korean Ministry of Food and Drug Safety on 22 Aug 2012, as the second-line therapy in metastatic RCC.
The aim of this post-marketing surveillance (PMS) study was to verify the safety and effectiveness of axitinib in Korean patients with advanced RCC. Within the limitation of phase IV study conducted as a part of a re-evaluation process, real-world outcomes of axitinib were evaluated in a large group of Korean patients treated in a clinical setting where therapeutic decisions are based solely on physician’s discretion. An advantage of such studies is the ability to capture more adverse events, including the rarer ones, along with some deviations from the effectiveness data obtained in generally smaller phase 3 patient sample size.
Materials and Methods
1. Study design and patients
The study was designed and conducted as an observational, phase IV PMS study of axitinib (product name: Inlyta) with a planned study period of 9 years. Eligible patients were required to be adult (aged > 18 years) patients with histologically-confirmed advanced RCC, failed to a prior first-line systemic therapy with tyrosine kinase inhibitors, and to have a measurable metastatic lesion(s). As this was an all-case PMS study, patients either who were already taking axitinib or who started taking axitinib during the study period were all invited to the study if the eligibility criteria were met. After obtaining a signed written informed consent, the patient was followed up until consent withdrawal, death, or the end of the study period, whichever came first. As per study protocol, safety follow-up data were collected from the day of first axitinib dose to up to at least 28 days after the last dose. Study-related data were collected from medical records and laboratory test results. As the study was designed as a multicenter, observational study under routine clinical practices, all clinical decisions, including the dosing and treatment duration of axitinib, were up to local clinical practice standards and the investigator’s clinical judgment.
As per prescription guidelines, it was recommended that second-line axitinib at a starting dose of 5 mg twice daily was administrated orally without interruption. Supportive care including the administration of blood products, and the use of analgesics was given if judged appropriately by the treating physicians. Treatment schedule, evaluations, and follow-up were judged at the discretion of treating oncologists. Axitinib was continued until disease progression, unacceptable toxicity, or consent withdrawal. Dose adjustments at the start of a new cycle were based on the worst toxicity observed during the previous cycle, in accordance with the AXIS trial protocol [5].
2. Evaluation variables
Patient’s demographic data, laboratory test results, axitinib administration details, concomitant medications, and tumor assessment results were collected during routine clinical practice. In addition, any observed or reported adverse events, regardless of the relationship with axitinib, were collected since the first dose of axitinib. The severity of an adverse event was graded according to the Common Terminology Criteria for Adverse Events ver. 5.0. Except for those of which causality was evaluated to be unlikely, all adverse events were attributed to axitinib. Tumor lesions were measured unidimensional according to the Response Evaluation Criteria in Solid Tumors ver. 1.1. The objective response rate (ORR) was defined as the proportion of patients achieving the best overall response of complete response or partial response. Progression-free survival (PFS) was defined as the time from the first dose of axitinib to the first documentation of objective tumor progression or death due to any cause, whichever occurred first. All study data were captured on the electronic case report form and monitored by the designated study monitors.
3. Sample size and statistical analysis
As the study was an observational study, the sample size was estimated based on the available target patients. At least 100 patients were to be enrolled and followed up for 9 years. Patients who received at least one dose of axitinib and had safety data were included in the analysis. Continuous variables were summarized with descriptive statistics, and categorical variables were presented with frequency and percentage. Adverse events were coded with the Medical Dictionary for Regulatory Activities (MedDRA) ver. 24.0. Although no formal comparisons between groups were planned, if needed, proportions between subgroups were compared using chi-square or Fisher exact test. Logistic regression analysis was performed to identify a factor affecting the ORR. A two-sided p-value less than 0.05 was considered to be statistically significant. Survival time was calculated using the Kaplan-Meier method. All statistical analyses were carried out with SAS ver. 9.4 (SAS Institute Inc., Cary, NC).
Results
1. Patient characteristics
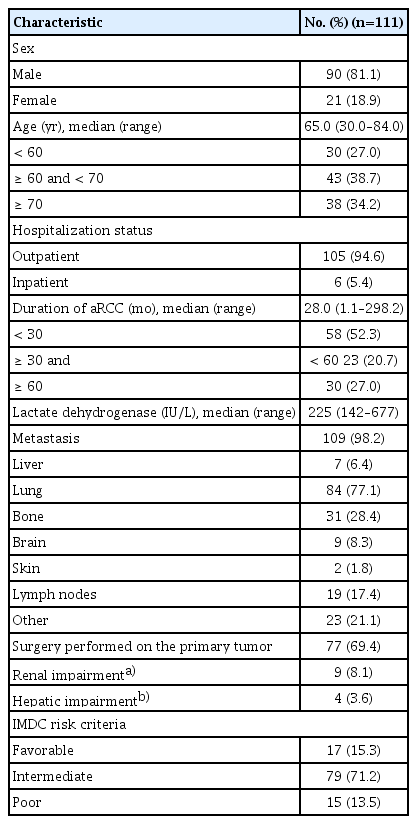
Among a total of 125 patients with advanced RCC enrolled between August 2012 and August 2021 21 hospitals in Korea, 111 patients were considered eligible for the present analyses. Reasons for exclusion included: (1) starting dose was different from the approved product label (n=10), (2) axitinib was given as third-line treatment (n=2), (3) patient refusal (n=1), and (4) no evidence of disease progression after first-line therapy (n=1). The majority (81%) of patients were male; age ranged from 30 to 84 years with a median of 65 years (Table 1). Except in one patient with histologically co-existing papillary type 2 and clear cell RCC, all were diagnosed with clear cell RCC. And as first-line of systemic therapy, the number of patients with sunitinib was 51 (46%), pazopanib was 57 (51%) and other treatment was 3 (3%), respectively. The median duration between the start of first-line systemic tyrosine kinase inhibitors and the time of axitinib treatment initiation was 28 months, and in 27% of patients, the duration was 60 months or longer. The most commonly involved metastatic site was lung (77%) and next was bone (28%). About 70% of patients previously received surgical resection of the primary tumor. The numbers of patients receiving prior immunotherapy or radiation therapy were one (0.90%) and 26 (23%), respectively.
2. Exposure to axitinib
Except in one patient, a treatment period of axitinib was available. The duration of axitinib administration ranged from 15 days to 25 months with a median of 5.6 months. About 48% of patients received axitinib for 6 months or longer. The median daily dose of axitinib was 10 mg (range, 4.36 to 15.95 mg). Axitinib daily dose was maintained at 10 mg in 65% of patients. Dose escalation of axitinib above 10 mg daily was possible in six patients (5%).
3. Safety of axitinib
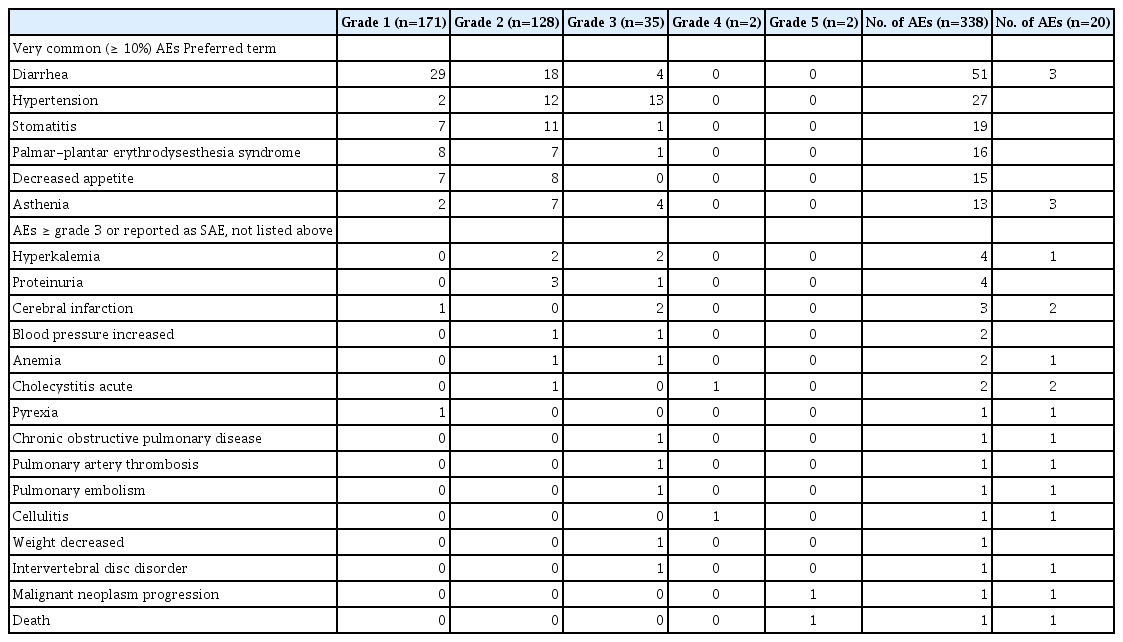
Ninety-two patients (83%) experienced 338 adverse events, 71% (264/338) of which were evaluated to be related to axitinib. Serious adverse events were reported in 14 patients (12%), and most adverse events were generally well tolerated and easily manageable. Most commonly reported adverse event was diarrhea (36%), followed by hypertension, stomatitis, decreased appetite, palmar-plantar erythrodysesthesia, and asthenia (Table 2). Axitinib dose was reduced in 20%, and axitinib was discontinued in 8% of the patients. Twenty-three unexpected adverse drug reactions were experienced by 16 patients (14%) (S1 Table), and none of them was reported as a serious adverse drug reaction. No statistical difference in the incidence of adverse events was found in the subgroups based on age or hospitalization status (Table 3). However, women had higher adverse event incidence than men (100% vs. 79%, p=0.021).
The proportion of severe (grade 3 or higher) adverse events was 12% (39/338) (Table 2). During the study period, two deaths were reported. One patient, a 75-year-old woman was found dead at home after 18 months of axitinib therapy. This event was thought unlikely to be related to study treatment because her disease remained stable and no serious adverse events were reported until then. Another patient, a 57-year-old man with multiple bone and brain metastases experienced disease progression and died 1 month after starting second-line axitinib. This event was considered to be not related to axitinib but to underlying disease.
4. Effectiveness of axitinib
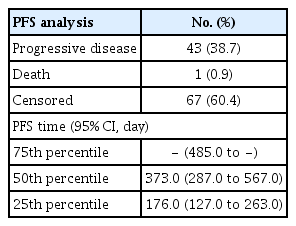
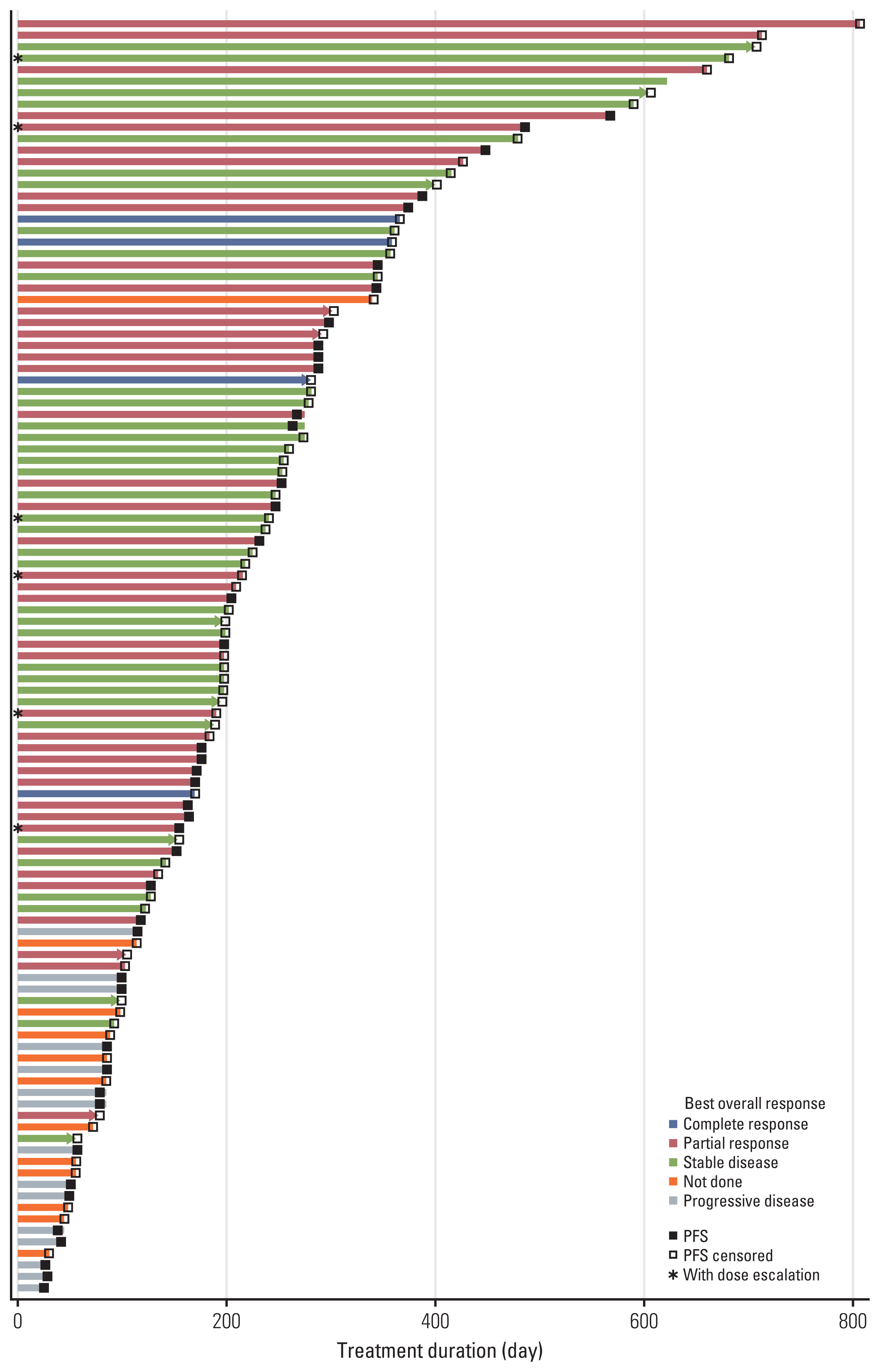
With a median follow-up duration of 8 months, the median PFS was 12.4 months (95% confidence interval [CI], 9.6 to 18.9) (Table 4, Fig. 1). The ORR was 30%, with 4% of complete response and 26% of partial response. No statistical difference in the ORR was found between the subgroups by demographics, baseline characteristics, concomitant medications, or axitinib doses (Table 5, S2 Table). However, patients with a shorter duration of axitinib administration had a worse ORR than the other two subgroups (10% [< 90 days] vs. 41% [90 to 179 days] or 36% [≥ 180 days], p=0.018). Multiple logistic regression analysis also showed that longer administration of axitinib was associated with a greater ORR with the odds ratio of 1.11 (95% CI, 1.02 to 1.20) (p=0.011). Of the total 111 patients, there were six patients who increased the dose at least one time. The overall treatment duration and ORR of all patients and patients with dose escalation were shown in Fig. 2, and the overall treatment duration and response were favorable despite of the dose escalation. In particular, among six patients who had at least one axitinib dose escalation event, two of them had relatively long-term duration of axitinib treatments, which were initiated following pazopanib as first-line therapy in both patients. One patient, a 66-year-old male, received axitinib with mean daily dose of 15.1 mg for 20.6 months and maintained stable disease while on axitinib treatment. The other patient, a 67-year-old male, received axitinib with mean daily dose of 16.4 mg for 14.9 months and had partial response till disease progress. Adverse events reported in both patients included dysphonia, diarrhea, and pruritus, which were all mild in intensity.
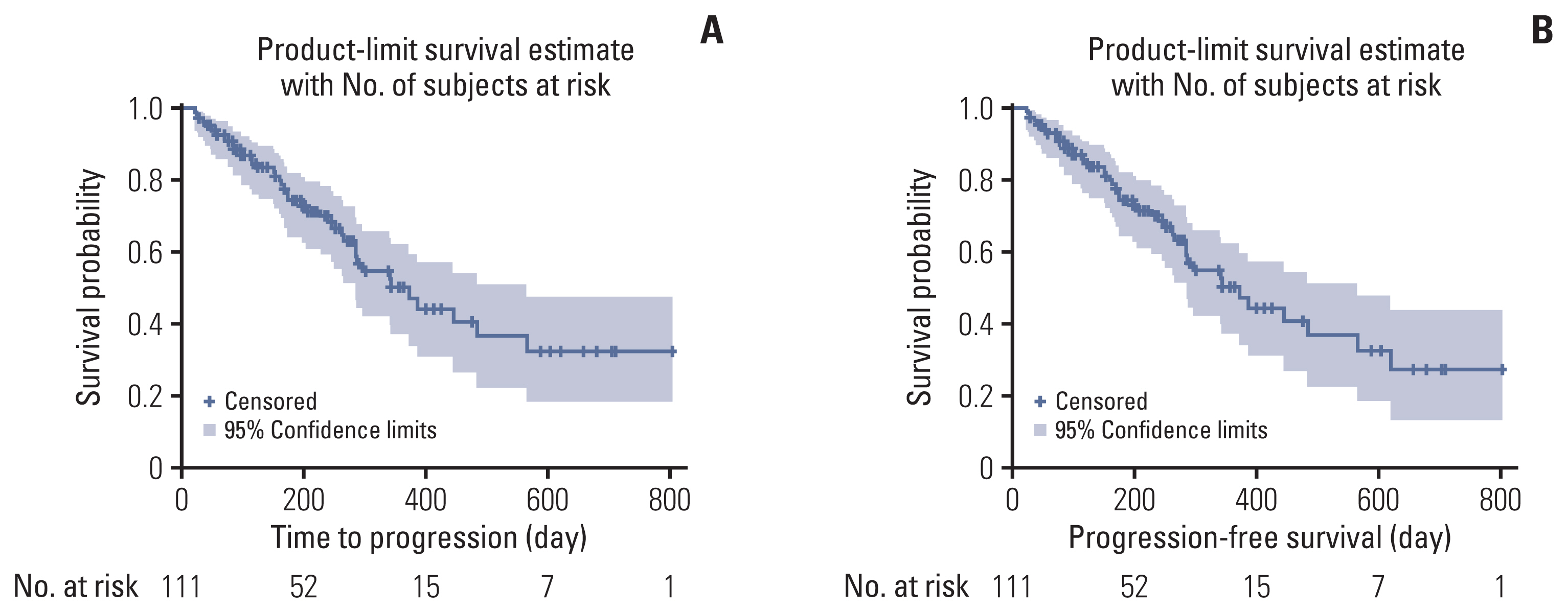
Kaplan-Meier curves depicting the time to progression (A) and progression-free survival (B) from the initiation of axitinib treatment in 111 patients with advanced renal cell carcinoma that did not respond to prior systemic therapy.
Discussion
This PMS study analyzed the safety and effectiveness of axitinib in Korean patients with advanced RCC. The results of this study add to the information obtained in the previous registration trial of axitinib [5,7,8]. Uncontrolled reports from PMS may provide us with a ‘real world’ data on axitinib complementary to the data obtained with strictly controlled phase 3 trials.
A total of 338 adverse events were reported in this PMS study of 111 patients, with 78% of the adverse events related to axitinib. A similar profile of adverse events was also reported in a randomized study comparing axitinib and sorafenib as second-line therapy in Asian patients with metastatic RCC [9]. The axitinib arm of the trial included 135 patients, mainly from China. The most common adverse events reported included hypertension (50%), weight decrease (37%), diarrhea (34%), palmar-plantar erythrodysesthesia (32%), decreased appetite (30%), hypothyroidism (28%), and fatigue (27%) 9. All these adverse events have also been frequently reported in the trials of RCC patients treated with other VEGFR inhibitors [10]. The incidence rates for specific adverse events in the present PMS study tended to be generally lower than those in the AXIS trial [5]. This might be associated with the fact that the present study was conducted in a less strictly controlled manner than the AXIS trial, and therapeutic decisions, including axitinib’s dose modifications, were based solely on physician’s discretion. However, the profile of the most common adverse events was essentially similar.
Median PFS in the present study was 12.4 months (95% CI, 9.6 to 18.9). This value is markedly longer compared with 6.7 months (95% CI, 6.3 to 8.6) in axitinib-treated patients participating in the AXIS trial [5] or 6.5 months (95% CI, 4.7 to 9.1) recorded in the Asian registration study of axitinib [9]. The ORR in the present study was 30%, with the vast majority of partial responses. This ORR was higher than the 19% ORR in the AXIS trial [5] and comparable with 24% in the Asian registration trial of axitinib [9]. We had about 14% of patients with IMDC poor risk RCC, less than those enrolled in AXIS trial. It is advised to recognize different patient population (i.e., number of risk scores), different study designs, and a potential biological variability between randomized phase III trials and real-world studies. Furthermore, no significant differences in the ORR were observed after stratifying the study patients according to their age. Also, the results of a recent real-world AXILONG study imply that some patients with RCC might benefit from second- and subsequent-line axitinib therapy more than previously supposed. In the AXILONG study [11], median PFS in a subgroup of patients with more favorable predictive factors (older age at the start of the treatment and baseline hemoglobin greater than lower limit of normal) was 18.1 months (95% CI, 13.8 to 22.5), with ORR of 46%, both figures being substantially higher than in the AXIS trial [5].
In the present study, the vast majority of patients received axitinib as the second-line therapy after treatment with a first-generation VEGFR tyrosine kinase inhibitor (TKI), sunitinib, or pazopanib. How-ever, new-generation immunotherapies have emerged recently as a promising first-line treatment alternative in advanced RCC. Simultaneously, a question arose which subsequent treatment should be offered to patients in whom these new generation immunotherapies failed. The results of two recent studies, involving patients with metastatic clear cell RCC, who received a subsequent TKI after the failure of therapy with the combination of two novel checkpoint inhibitors, nivolumab+ipilimumab, suggest that axitinib could be considered a second-line treatment option in this setting as well [12,13].
This study has some limitations that restrict the interpretability of its results. Most importantly, the analysis did not include some clinical variables that might affect the effectiveness outcomes of axitinib, including the prior response to first-line therapy. While these limitations should be considered during the interpretation of the results, also the strengths of the study related to its real-world character and large sample size are worth emphasizing.
Taken altogether, the results of this PMS study demonstrated that in a ‘real world’ setting, axitinib provides a valid second-line treatment option for Korean patients with advanced RCC and that the safety and effectiveness of this drug in the Korean population are consistent with previous reports from registration trials [5,7].
Electronic Supplementary Material
Supplementary materials are available at Cancer Research and Treatment website (https://www.e-crt.org).
Notes
Ethical Statement
The study was conducted in accordance with the local regulations and Good Pharmacoepidemiology Practice guidelines. The study protocol was reviewed and approved by the Korean MFDS and institutional review boards of all participating hospitals. Informed consent was obtained from all participants before study-related data was collected.
Author Contributions
Conceived and designed the analysis: Shin SJ, Park SH.
Collected the data: Shin SJ, Lee JL, Kwon TG, Shim BY, Chung HS, Park SH.
Contributed data or analysis tools: Shin SJ, Lee JL, Kwon TG, Shim BY, Chung HS, Kim SH, Park SH.
Performed the analysis: Shin SJ, Kim SH, Park SH.
Wrote the paper: Kim SH, Park SH.
Conflicts of Interest
Sang Joon Shin, Jae Lyun Lee, Tae Gyun Kwon, Sang-Hee Kim, and Se Hoon Park have received research grants for this study from Pfizer. SH Kim is full time employ of Pfizer Pharmaceutical Ltd. The authors have no other relevant affiliations or financial interest in or financial conflict with the subject matter or materials discussed in the manuscript apart from those disclosed.
This study was sponsored by Pfizer Pharmaceuticals Korea Ltd.
Acknowledgments
All investigators participated in this study are listed as below. Study sites were written at the time of study in alphabetical order. Ho Seok Chung (Chonnam National University Hwasun Hospital), Hee Jun Kim (Chung-Ang University Hospital), Seok Joong Yun (Chungbuk National University Hospital), Hyo Jin Lee (Chungnam National University Hospital), Ho Young Kim (Hallym University Sacred Heart Hospital), Sung Yul Park (Hanyang University Medical Center), Joo Han Lim (Inha University Hospital), Jae Il Chung (Inje University Busan Paik Hospital), Byeong Hun Kim, Jin Yeong Kim (Keimyung University Dongsan Medical Center), Jong Gwon Choi (Konyang University Hospital), Jae Young Park (Korea University Ansan Hospital), Seong Hoon Shin (Kosin University Gospel Hospital), Tae Gyun Kwon (Kyungpook National University Chilgok Hospital), Ja Yoon Ku (Pusan National University Hospital), Se Hoon Park (Samsung Medical Center), Jae Lyun Lee (Asan Medical Center), Koung Jin Suh (Seoul National University Bundang Hospital), Sang Joon Shin (Severance Hospital), Hye Rim Ha (The Catholic University of Korea, Incheon St. Mary’s Hospital), Byoung Yong Shim (The Catholic University of Korea, St. Vincent Hospital), Hae Su Kim (Veterans Health Service Medical Center), Seng Taek Lim (Yonsei University Wonju Severance Christian Hospital), Ill Young Seo (Wonkwang University Hospital).